Last Updated on September 28, 2022 by Rebecca Huff
How quickly can you increase ferritin levels? With the method outlined below, it's possible to improve iron stores in 6-8 weeks, depending on why you are deficient.
If your blood levels are low due to menstruation, it may take longer. Menorrhagia, depending on the severity can make it difficult, and sometimes impossible to achieve normal ferritin levels. Heavy bleeding may even lead to a blood transfusion. Because low iron levels or severely low levels of ferritin can cause chest pain or even heart failure.
This is why it's crucial to keep an eye on iron and ferritin levels, especially if you have blood loss, such as with menorrhagia or celiac disease. Iron is an essential mineral because it is needed to make hemoglobin, a part of blood cells that carries oxygen throughout the body.
Your doctor can order a blood test called a complete blood count (CBC) to check red blood cell counts, hemoglobin or hematocrit levels. Other lab tests such as serum iron can check ferritin levels.
The total iron–binding capacity (TIBC) test looks at how well the iron moves through your body. Iron is an important mineral that your body needs to stay healthy.
Keeping total iron in the normal range is important as high ferritin can be dangerous as well.
What is Iron Deficiency?
I've dealt with iron deficiency, iron-deficiency anemia, and low ferritin levels on and off since my first pregnancy. It is easy for doctors to overlook or misdiagnose. Briefly
- Iron deficiency means the body lacks iron.
- Iron-deficiency anemia is a lack of iron as well as Hemoglobin.
- Low ferritin – Ferritin is a protein containing iron and is the main form of iron stored inside of cells. The small amount of ferritin that is discharged to circulate in the blood is an indication of the total amount of iron stored in the body. (Ferritin stores iron and moves it through the body to where it is needed.)
- Iron deficiency without anemia is similar to iron deficiency in that the body is lacking iron but has normal hemoglobin levels. Iron deficiency without anemia is a late manifestation of iron deficiency. “Weakness, fatigue, difficulty in concentrating, and poor work productivity are nonspecific symptoms ascribed to low delivery of oxygen to body tissues and decreased activity of iron‐containing enzymes.” (1)
- Anemia without iron deficiency can happen for a variety of reasons. One, in particular, would be pernicious anemia which happens when the body can't make enough healthy red blood cells because it doesn't have enough vitamin B12. (2)
Misdiagnoses often include anxiety, depression, chronic fatigue, cardiac or pulmonary issues. Many people, including myself, may experience chest pain severe enough to warrant a trip to the ER due to iron deficiency.
The symptoms of low iron (all versions) are:
- Blue sclera (white part of eyes can take on a bluish tint, similar to the look of skim milk)
- Chest Pain
- Cold hands and feet
- Depression
- Dizziness/lightheadedness
- Fainting
- Fatigue
- Hair Loss
- Headaches
- Irregular heartbeat or heart palpitations
- Irritability
- Pica (a persistent pattern of eating non-food items including ice, glue, paint, sand, dirt, clay, starch, etc.)
- Pallor or pale skin (oxygen-rich blood is scarce and is being diverted away from the skin to major organs)
- Light areas inside of the eyelids, mouth, and cheeks
- Whitish and sore tongue
- Pounding or “whooshing” in your ears
- Sensitivity to cold (low body temperature, unable to get and stay warm)
- Shortness of Breath after simple tasks such as climbing stairs, walking short distances, doing housework
- Tachycardia (rapid heartbeat)
- Weakness
- Restless Legs Syndrome (RLS) (tingly or twitching legs that move uncontrollably, especially at bedtime)
- Skin color can be a gray-green or pale yellow
- Brittle nails, or nails with ridges or depressed areas
Who is iron deficient?
Pregnant women and those who have heavy menstrual cycles may have an iron deficiency. Often women have increased blood loss due to fluctuations in hormones during peri-menopause. Blood donors typically lose between 220-250 mg of iron at one donation, not usually a problem for men, but it's something women need to consider.
Cancer patients may require iron infusions. Gastrointestinal bleeding may result in iron deficiency.
Those with hepatitis B may have iron overload.
You can find out using a home Iron, TIBC, and Ferritin panel at home or asking your doctor to do this test for you.
In addition, some people carry a gene, TMPRSS6, which regulates a protein that controls how much iron you absorb from food. At rs4820268, the ‘G’ allele is associated with lower blood iron levels. You can find out if you have such a gene with a simple home genetic test kit, like the one I used from SelfDecode.
Read my review here Genetic Testing at Home – My Review of SelfDecode.
Ditching Iron Supplements
I was blessed to meet a kindred spirit in Sarah Galbraith Laucks who gave me the following instructions on how to increase my iron naturally.
During our conversations, we happened to find out that we had both experienced similar health challenges. One of which, was iron deficiency. While I had used iron infusions to get my levels up, Sarah had researched and implemented natural strategies to correct her deficiency.
This impressed me because I knew that the iron infusion solution is just a bandaid. It doesn’t get at the root at all. I know this for a fact because I've had multiple iron infusions, prescribed by my functional medicine doctors.
Conventional doctors always took the iron supplement route, prescribing ferrous sulfate. Sadly, I found that iron supplements just don’t work. In addition, iron supplements nauseated me every day, not to mention constipation they cause.
I asked Sarah to share everything she did to improve her iron and thankfully, she agreed! The section below is what she advised for me, followed by the results I got from following her advice.
Increasing Iron Levels
by Sarah Galbraith Laucks
Here is the list of what I did to resolve my issues. The three core things that I feel solved the problem.
1 Eat Iron-Rich Foods or Pills Containing Them
Eating iron-rich foods is advised, however many people aren't able to tolerate these foods.
All the research said if you want to fix the problem (when it’s iron-deficient anemia) Beef Liver is the answer. I couldn’t tolerate eating it because I:
- Don’t know how to cook it right, and
- Am not used to eating it.
My solution was to take at least 6 Beef Liver pills every day. I ended up using the Ancestral Supplements brand.
I feel their product is best for a variety of reasons. (More on this at the bottom of this article.) I alternated with their Beef Spleen Pills to boost my heme iron levels because the spleen has five times the amount of iron as the liver does.
Spleen and Bone Marrow Supplements
Even though the spleen has more iron than the liver, the liver is the core treatment because it has the total package. There’s more A in beef liver than any other food source, and by a long shot. Even though most say you need Vitamin C to boost iron uptake, the reality is that you need Vitamin A. European doctors talk about this all the time. For some reason, it’s lost here in the USA.
I also took 3-6 Bone Marrow pills each day, again from Ancestral, to boost bone marrow production because with anemia part of the issue is the bone marrow isn’t producing strong red blood cells. Following the “like supports like” principle here.
I also made a lot of chicken broth – mostly meat stock. From chickens who had been laying hens. I drank 1-2 cups per day. Also, I ate a lot of chicken livers which I found I loved.
I buy liverwurst from US Wellness Meats – that’s a great way to get beef liver. I’m currently teaching my 9-year-old to love it. Plus, I ate red meat at least every other day, every day if I could.
2 Boost Vitamin A
Fermented Cod Liver Oil from Green Pastures is critical, because of the Vitamin A content. I use the version that has the butter oil in it and take 1/2 teaspoon 3x a day (with every meal). A very big part of resolving this issue is boosting Vitamin A and boosting it a lot. Everything I read from Europe and all the functional medicine people I talked to basically said: “Oh yeah, those Americans, they are SO deficient in Vitamin A.” It was like a joke to them. The Europeans all know better. They all eat organs, or fish eggs, on a regular basis. Me? I was eating none of that lol, so no surprise I had issues!
3 Practice Grounding

Grounding is connecting to the electrical energy present on the surface of the planet. I ground 24/7. The moment I started grounding my numbers began to improve. Literally. I had blood work done, then 2 weeks later started grounding, then 2 weeks after that had more bloodwork. My doctor was on the verge of giving me an iron infusion and then saw the bloodwork and said “no, I think we can wait.”
Earthing is an excellent film that just came out, which you can watch for free that explains the concept. Read The Earth Prescription in which holistic physician Laura Koniver, MD, offers the ideal antidote to the toxicity of a life isolated from nature—grounding, or directly touching the earth to heal your body and rejuvenate your sense of total well-being. Earthing will allow you to tap into the Earths natural energy.
If I am inside I am grounded. Sleep with grounding sheets. When at the computer I have my bare feet on a universal grounding mat. Outside I am barefoot.
The reason is that grounding is proven in really excellent studies to:
- Improve blood flow (viscosity) – so the blood gets where it needs to go in a better fashion, improve blood oxygenation (which means stronger, healthier red blood cells which I felt probably meant they would carry nutrients better as well)
- Supports vagal tone (complicated to explain why this helps, but it does and is important), and improves bone marrow’s ability to produce cells (red and white blood cells).
Putting it all together – Rebecca's experience
When Sarah shared her list with me, I was excited to get started. My blood tests at the time show my ferritin levels were well below the lower limit. I didn't need the labs to tell me because my muscles burned when I did the simplest everyday activities. Climbing the stairs to my apartment was like being on a machine at the gym for hours.
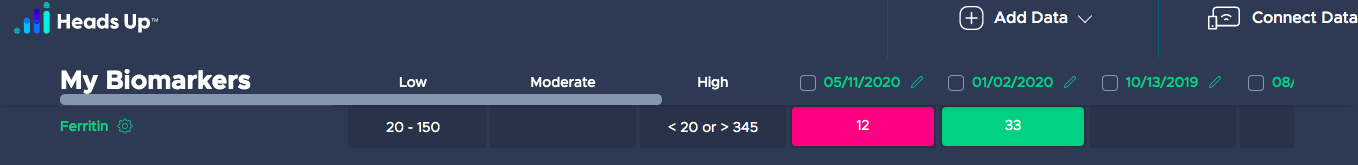
For the first month, I took six Beef Liver pills from Ancestral Supplements daily. In the second month, I rotated with the Beef Spleen pills. According to Ancestral Supplements:
Spleen has five times more heme iron than liver. With 12.5 MG of heme iron per serving, spleen is the most concentrated source of heme iron that exists in nature. If you're looking for iron, look at the Grass Fed Spleen supplement.
My chances of increasing my iron intake from food sources enough to tip the scale are low, considering my test results. While I believe dietary iron is the most natural way to get enough iron in my body, I have no intention of eliminating my Beef Liver pills, since they are 100% freeze-dried liver. I aim to eat liver at least once per week because animal-based iron is more readily absorbed while plant-based sources are less bioavailable.
Of course, it's always a good idea to consume a variety of sources of iron including both heme and non-heme iron. Although non-heme iron absorption can depend on a variety of factors including inhibitors such as phytic acid and polyphenols in vegetables, grains and legumes.
I added beef liver as well as marrow bones from Farm Foods to my diet. The marrow bones are delicious, I roast them in a skillet or salt block and eat the marrow before using the bones for beef broth.
My daughters have had low iron on and off due to heavy periods. Our doctor recommended red meat, which we source from farms who raise grassfed and finished products, such as:
- Butcher Box
- Snake River Farms
- Farm Foods (use coupon code WELCOME to save 10%)
Based on the concept of “like supports like,” consuming bone, marrow and cartilage may strengthen and support our own bone, marrow and cartilage health.* Whole bone extract and marrow naturally provides all the nutrients (collagen, growth factors, stem cells, fat-soluble activators, trace minerals, etc) that support bone, dental and connective tissue health.
To cover my bases, I also supplement with Ancestral's Beef Bone Marrow pills.
Iron Absorption
An individual's absorption of iron from foods will depend on multiple factors, such as overall digestive health and the quality and variety of foods eaten. My body needs help with digestion, as do many people my age. For this, I supplement with Ancestral Supplements Pancreas, following the like supports like concept again.
Results
Currently, my iron status is improving. My doctor agrees that I no longer need an iron-infusion. Which I'm grateful for because my insurance company no longer covers them. The out-of-pocket cost for me would be over two-thousand dollars. That makes beef liver pills seem cheap in comparison, no?
Dietitians recommend eating iron-rich foods along with Vitamin C; based on Sarah's research, I add Vitamin A-rich foods to that list.
Iron Foods and Helpers (that contain vitamins A or C and increase iron absorption)
- orange juice
- lentils
- apricots
- dried fruit
- dark green leafy vegetables such as kale
- prunes
- clams, mussels
- bell peppers
Foods that block iron
Breakfast cereals are often iron-fortified however, even though many contain whole grains, they are not typically considered health food. Whole grains are a phytate-containing food that also blocks the absorption of iron. This phytate and iron combination can undermine your efforts to correct iron deficiency.
Dairy products, coffee, tea, chocolate, eggs, and fiber can prevent iron absorption due to the tannins. Avoid combining iron-rich foods with calcium-rich foods, as calcium binds to iron, which will hinder iron absorption. Check multiple vitamins or other combination supplements for iron and calcium combinations.

Sarah Galbraith Laucks
For more than 20 years I've been exploring wellness strategies that are effective for me and others. I've tried all manner of eating protocols, fitness programs, and therapies. I've discovered that the standard approach doesn't work for everyone and how important it is to understand our own unique bodies to determine how we can be as healthy as possible.
These days I'm focused on ways to be well that are simple, affordable, and produce results. Currently obsessed with: biohacking, grounding, isometrics, and eating as clean as possible. In my professional life, I am a nationally recognized expert in the planning of conferences and events that are accessible for people with disabilities. I also help women-owned small health and wellness businesses with their marketing.
Follow Sarah's adventures on Instagram.
Updated April 3, 2022
When supplementation and food sources aren't enough
I've revisited this article again due to my daughter having extremely low iron brought on by a heavy menstrual cycle. While eating leafy greens, legumes, and other good sources of iron, she still was only able to improve by five points over three months. Her iron deficiency was caused by blood loss therefore we first needed to address that problem, then tackle the side effects which were low iron and fatigue. (Shortness of breath, fatigue, and exhaustion are symptoms of iron deficiency that make it incredibly hard to exercise while anemic.)
Because her ferritin levels were dangerously low, she did have an iron infusion. (Injectafer is the best source of intravenous iron replacement that we have found when levels are critically low. Compared to other types of iron infusions, it has the least side effects and she was able to go on with her life right after the infusion.)
It is also important to note that anyone supplementing with iron should work with a health care provider to establish a safe and effective plan. High iron (hemochromatosis) can be dangerous so it is crucial to monitor iron and ferritin levels with regular lab tests. (Ask your doctor to check not just your iron but also your serum ferritin to determine how well your body stores iron. Your doctor might run a TIBC or Total Iron Binding Capacity panel which measures transferrin – how well the transportation of iron in your body is working.)
Other information on iron deficiency
To read more about Rebecca's journey and past posts about the treatment methods I've tried for improving iron:
Disclaimer: Consult with your personal healthcare provider before implementing any changes to your diet or supplement regimen.
Sources:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5986027/
- https://www.health24.com/Lifestyle/Your-Blood/Anaemia-20130216-2
- Mayo Clinic – https://www.mayoclinic.org/diseases-conditions/menorrhagia/diagnosis-treatment/drc-20352834
- https://www.urmc.rochester.edu/encyclopedia/content.aspx
- Gasche, C et al. “Iron, anaemia, and inflammatory bowel diseases.” Gut vol. 53,8 (2004): 1190-7. doi:10.1136/gut.2003.035758





 Old Fashioned Stack Cake Recipe
Old Fashioned Stack Cake Recipe
Thank you! I have had anemia on and off for most of my life. Pills have never helped, I eat clean, organic, well rounded gluten free (celiac) dairy free, grain free (too harsh with my celiac), and I’ve been on all kinds of iron supplements. Iron supplements do not work, nothing happens. For 40 years the best that works is lots of greens. Lately I’m dragging myself with no relief. Putting all your suggestions into practice
I’m the same as you, the iron pills didn’t work. It’s unfortunate that it requires so much work to keep iron levels up, but that’s just the reality for some of us. I have to monitor mine closely. Hope you have success!